Insulin pumps and pods can help people with diabetes take control of their disease. Continuous subcutaneous insulin infusion with or without continuous glucose monitoring provides tight blood glucose control. It lower hemoglobin A1c compared to traditional injection methods. When combined with continuous glucose monitoring, these devices can reduce the risk of hypoglycemia. Unfortunately, there are some drawbacks to insulin pump and insulin pod adhesives. One of the more challenging issues is when the skin reacts to the pump’s adhesive. We will discuss the challenges of using insulin pumps and insulin pods, and practical ways to manage skin reactions.
First, the benefits of using insulin pumps and insulin pods
Glucose monitoring and insulin infusion devices have come a long way since they were first introduced. The devices have earned the name “artificial pancreas” because they now do what the endocrine pancreas does, sense glucose levels and provide insulin (future models may also provide glucagon) when a person needs it. When properly programmed, insulin pumps and insulin pods can eliminate the need for insulin shots, provide better glucose control than most people can achieve with insulin shots, and may guard against low blood sugar. People can eat and exercise as they please because the devices can adjust insulin infusion to circulating glucose levels.
To make glucose and insulin management more convenient, some devices are combined with glucose monitors or continuous glucose monitoring. The DANA Diabecare IISG insulin pump and Insulet Omnipod device have integrated glucose meters. Animas Ping operates in a similar way, though the pump and glucose meter can function independently. The Animas Vibe integrates the Dexcom G4 Continuous Glucose Monitor with an insulin pump, and the Medtronic Diabetes Minimed Paradigm pumps wirelessly communicate information between pump and glucose meter or Continuous Glucose Monitor. The MiniMed 670G operates on a closed-loop system, acting as nearly a true “artificial pancreas.”
Now, the drawbacks of insulin pumps and insulin pods
First, the devices are expensive. While insulin itself is certainly not cheap, the devices and ongoing costs for service and supplies can add up. The devices can be difficult to program and difficult to use without training and practice.
Many people with diabetes find the devices cumbersome, heavy, and uncomfortable. While it may be an “artificial pancreas,” it is an organ that you now wear on the outside of your body virtually all the time. This means wearing it in the shower, while exercising, when you are trying to sleep, and on occasions where you don’t want a visible reminder of your diabetes.
While you no longer have to inject insulin, the devices still infuse insulin through a needle or a cannula. The needle, while a rather painless one, usually, is still another needle. If the device has a cannula, the number of breaks in the skin are fewer, but the tube can become kinked or dislodged. While you can avoid traditional needle injections, most people still check their blood glucose by fingerstick a few times a day, just to make sure the insulin pump and insulin pod is working properly.
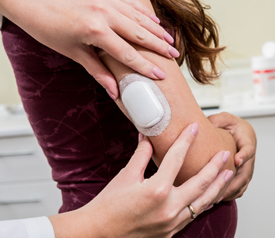
Lastly, these devices stick to your body by adhesive. Patients often develop allergy-like skin reactions to the adhesives in insulin pumps and insulin pods. In fact, some people stop using the devices because the skin reaction is intolerable.
Ways to deal with skin reactions to adhesive in insulin pods and insulin pumps
A quick look through diabetes patient forums reveals countless posts about skin reactions to the adhesive in insulin pods and insulin pumps. Certainly, people with latex allergy have immediate difficulty with some devices, but even people who have never struggled with allergy can develop one over time. The reactions can be severe; people who have used insulin pumps without problem for over a decade have found themselves needing to go back to shots because the adhesive allergy is so terrible.
The first step in treating any skin allergy or skin reaction is to remove the offending agent. Unfortunately, in the case of insulin pump and insulin pod, the adhesive is integrated into the device itself. People have tried moving the device to a new location on the body to allow the skin eruption to heal. This works, temporarily, until the new location becomes inflamed. While going back to shots or changing insulin infusion devices may be the definitive solution for insulin pump skin allergy, it is not always practical. Especially if the person has gotten comfortable with a particular device (programming, filling, monitoring, etc.)
A deeper dive into the diabetes forums show the lengths that people will go to keep their current device even though the adhesive is causing a reaction. Many have tried oral antihistamines, but anecdotally these seem ineffective. Several people have found relief from hydrocortisone spray or other topical corticosteroid. These drugs have powerful anti-inflammatory properties and certainly may work over the short term. However, constant use of steroid sprays or creams can cause atrophy of the skin, striae (i.e. stretch marks), spider veins, and acne. People can even develop an allergic reaction to the steroid itself.
Another approach is to use an alternative adhesive, different than the one provided with the insulin pump and insulin pod. Practically speaking, the patient leaves the backing on the device’s adhesive and covers the device with transparent dressing or medical tape. Many people have been able to block the skin reaction with this approach. However, it is critical that the pump and glucose monitor be securely fastened to the skin. Diabetic ketoacidosis and other reactions have occurred because insulin pump cannulas have become dislodged.
Hy-Tape provides insulin pump securement
Hy-Tape is an excellent choice to secure continuous glucose monitors, insulin pumps, and insulin pods. The Original Pink Tape® contains a latex-free, zinc oxide-based adhesive that is soothing to skin. While the adhesive is gentle on skin and removes cleanly, it also holds strong until you are ready to replace your device.
Instead of taking the backing off the adhesive that comes with the insulin or glucose monitoring device, leave it on, and use it as a guide to apply Hy-Tape around its border. The backing will protect the device’s adhesive from touching the skin, and Hy-Tape will hold the device securely in place. Hy-Tape comes in rolls and strips and is thin enough to conform in difficult to tape areas. That means it’s easy to apply, easy to remove, and holds strong. The Original Pink Tape® is also waterproof and resists soiling; so, if your insulin pump can handle a situation, so can Hy-Tape. Contact us for a free sample of Hy-Tape to try with your insulin pump and insulin pod. You may be able to keep using your current insulin pump or insulin pod.

