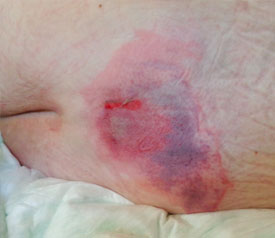
Sacral pressure ulcers are caused when bone pinched the overlying tissues. The pelvis, hip or lower spine are usually to blame (i.e., ischium, greater trochanter, or sacrum). When the patient’s body weight rests on one of these bones, it compresses the tissue and prevents blood from flowing to the area.1 Over time, the tissue becomes ischemic and begins to break down. While most sacral pressure ulcers are considered avoidable, they still occur. If a sacral pressure ulcer does happen, it must be dealt with quickly, vigilantly, and competently.
Assessing sacral pressure ulcers
Pressure-induced skin and soft tissue injuries are often classified using the National Pressure Ulcer Advisory Panel (NPUAP) staging system (recently updated in 2016). Under this rubric, the wound should be staged to its deepest extent. This means selecting the highest number stage that accurately describes any part of the wound.
- Stage 1 Pressure Injury: Non-blanchable erythema of intact skin
- Non-blanchable is redness that stays despite applying pressure. This means the erythema is not caused by blood within capillaries (which would be blanchable). Purple or maroon discoloration is not part of stage 1, but rather indicates a deep tissue pressure injury.
- Stage 2 Pressure Injury: Partial-thickness skin loss with exposed dermis
- In this stage of pressure ulcer, the epidermis is missing in places, which exposes the dermal layer (but not fat, fascia, bone, etc.). The wound bed is viable, and there is no granulation tissue, slough, or eschar present in the wound. Importantly, Stage 2 should not be used to describe moisture-associated skin damage such as medical adhesive-related skin injury (MARSI) or traumatic wounds (e.g. burns, abrasions).
- Stage 3 Pressure Injury: Full-thickness skin loss
- In this stage, the entire covering of skin is gone (epidermis and dermis), and fat is exposed. Other underlying tissues beyond fat are not exposed, however. The ulcer may include granulation tissue, slough, and/or eschar. The visible areas of the wound may have recesses (i.e. undermining and tunneling).
- Stage 4 Pressure Injury: Full-thickness skin and tissue loss
- Stage 4 is reserved for pressures ulcers in which tissues deep to fat are exposed such as fascia, muscle or bone.
Management of sacral ulcers varies by ulcer stage
It is important to properly stage pressure ulcers for several reasons, but two of the most important are for prognosis and management planning. Stage 1 and stage 2 pressure ulcers heal by regenerating tissue in the wound. Stage 3 and stage 4 pressure ulcers, on the other hand, heal through scar formation, which means the borders of the wound contract as it heals.
For Stage 1 sacral ulcers, the primary goal of therapy is to ensure adequate tissue perfusion and to protect the wound from further damage.2 This means preventing the sacrum from chronically squeezing the skin and preventing blood flow to the area. The goal of therapy for Stage 2 ulcers is to encourage tissue regeneration and protect the wound surface. For stage 3 or 4 ulcers, management efforts are focused on promoting tissue granulation and epithelialization.
Factors that influence sacral ulcer management
While wound management is a key part of sacral ulcer management, treating patients holistically is the key to success. Apart from ischemia, other factors that impede normal healing include poor nutrition, infection, edema, persistent moisture, fecal and urinary soiling, and shearing forces. One can look for, prevent, or minimize each of these risk factors. Of course, the patient should be frequently repositioned to avoid further tissue damage and to promote healing.
When selecting a dressing, the wound should be kept moist but not contain excessive amounts of exudate. Wound care professionals should consider the type of ulcer (arterial vs. venous vs. neuropathic) and any comorbid conditions that could complicate treatment (e.g. diabetes). Arterial wounds generally require a moisture-retaining dressing, while wounds that arise from venous insufficiency usually require a dressing that absorbs excess moisture. All surfaces of the wound, including any tunnels, should be packed with the appropriate dressing.
Selecting the right dressing for sacral ulcer management
A tremendous number of dressings are available for different types of wounds, and various guidelines are available to help wound care professionals determine which type of dressing should be used in various circumstances. For example, petrolatum-impregnated dressings are nonadherent dressings that are useful in wounds with minimal exudate. Conversely, alginates and hydrofiber are moderately or highly absorbent, respectively, which makes them useful in wounds with excessive exudate production.
Selecting the right medical tape for sacral pressure ulcers management
While substantial guidance is available for dressing selection, most clinical guidelines fail to discuss the importance of medical tape in sacral ulcer management. Sacral ulcers pose unique challenges in wound management, and the medical tape must be up to the task. Sacral ulcers are often subjected to excessive moisture and soiling from perspiration, urine, and fecal matter. The sacral area is subject to substantial friction and shear forces, as well. Each time the patient repositions themselves (or caregivers manually reposition patients), the sacral area takes the brunt of this movement. Lastly, the sacral region is not uniform in shape. And sacral ulcers also tend have irregular borders. Dressings must be cut to fit the wounds, and tape must be able to provide a secure border on all sides.
While various medical tapes are available to treat pressure tissue injuries, Hy-Tape is perhaps the best medical tape for treating sacral pressure ulcers. Hy-Tape is thin and flexible, which allows it to conform to the curvatures of the sacral area and the unique perimeters of sacral wounds. The adhesive found within Hy-Tape adheres more strongly as it warms with body temperature. Thus, Hy-Tape actually holds to peri-wound skin better when patients are lying supine and/or immobile. Moreover, Hy-Tape is occlusive and waterproof. Even though sacral wounds are prone to excessive moisture and soiling, Hy-Tape holds strong in this environment. The tape is even washable, so wound care professionals can bathe patients and clean soiled skin and linens while leaving dressings in place. When it is time for dressing change—which is frequently needed in patients with sacral ulcers—Hy-Tape releases cleanly and without residue. Perhaps more importantly, since sacral wounds are associated with tissue edema and moisture-related skin maceration, Hy-Tape releases gently without traumatizing macerated or friable skin.
If you care for someone who has or is at risk for sacral pressure ulcer, contact Hy-Tape for free sample.
References
1. Therattil PJ, Pastor C, Granick MS. Sacral pressure ulcer. Eplasty. 2013;13:ic18-ic18.
2. Bryant R, Nix D. Acute and chronic wounds: Current management concepts. Elsevier Health Sciences; 2015.

