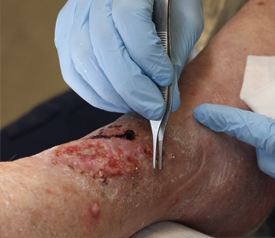
Introduction to Lower Extremity Wounds
Lower extremity wounds are very common, with an estimated prevalence of 1% to 2% among adults in the United States. These wounds have a profound effect on public health and patient outcomes. They are often complex and chronic wounds. Even when the best care available is applied, approximately 25% to 50% of leg ulcers and more than 30% of foot ulcers remain unhealed after six months of treatment.
There are multiple types of lower extremity wounds, including diabetic foot ulcers and those caused by venous or arterial insufficiency. There are also wounds with mixed etiology. The annual costs associated with venous leg ulcers and diabetic foot ulcers in the United States are approximately $14.9 billion and between $9 billion and $13 billion, respectively. These figures represent a huge burden on the national health care system. In addition to this, the cost of these wounds to patients is high, too. They often require more medical resources, miss more workdays, are hospitalized more frequently, and have more emergency department visits than other patients.1
While these wounds share many of the same risk factors, it’s a good idea to understand their differences, which can help clinicians develop more effective treatment outcomes.
Understanding Lower Extremity Wounds
Venous Ulcers
Venous leg ulcers (VLUs) are one of the most chronic types of leg wounds, and they can be incredibly challenging to treat. These wounds represent up to 70% of all chronic leg ulcers, particularly across the elderly population, which has an annual VLU prevalence of 1.7%.
VLUs develop when the valves in the leg veins are damaged, or the veins are dilated. Retrograde blood flow results in venous hypertension. Sustained venous pressure causes edema and extravasation of red blood cells that result in hemosiderin deposition and pigmentation. Mechanical disruption of the endothelial cells results in margination and the activation of white cells. The cumulative effect is persistent inflammation, oxidating stress, and the expression of multiple cytokines and chemokines. The overexpression of matrix metalloproteinases destroys dermal tissues and results in the formation of an ulcer. Growth factors become trapped by pericapillary fibrin cuffs, which disrupt the diffusion of oxygen, resulting in localized hypoxia. The ulcer then will remain open and draining, frequently surrounded by slough and induration.1
These ulcers frequently occur over the medial aspect of the lower leg between the lower calf and the medial malleolus. They may be pigmented, edematous, or contain venous dermatitis, atrophie balance, and lipodermatosclerosis. Many patients feel aching or burning pain that is alleviated with leg elevation.1 Infection is a tremendous concern, and additional complications are frequent, including delayed healing, cellulitis, wound enlargement, pain, and systemic illness.
Arterial Ulcers
Arterial ulcers are also a common type of lower extremity ulcer, representing approximately 10% of leg ulcers. These wounds are often painful and prone to infection and necrosis. They are caused by the lack of tissue oxygenation secondary to arterial obstruction of the lower limbs. In most cases, the cause is atherosclerosis.4 The decreased arterial blood flow contributes to the development of ischemia and impaired oxygenation. Extramural strangulation and mural thickening also contribute to reduced perfusion.1 While this initially results in intermittent worsening during exercise, as the disease progresses, poor perfusion becomes persistent, even while at rest. The damaged tissue will eventually ulcerate.
Arterial ulcers are common across patient populations, such as those who have diabetes, hyperlipidemia, hypertension, or those who smoke. They are also more common in elderly patients, obese patients, and those who have a sedentary lifestyle. Genetic risk factors include heart disease, cerebrovascular disease, or peripheral vascular disease in the family history.1
Arterial ulcers are often accompanied by resting pain at night. They will generally have a punched-out appearance with well-demarcated edges and a pale, nongranulated (and sometimes, necrotic) base. The periwound area is often erythematic, hairless, shiny, and friable.
Diabetic Foot Ulcers
Diabetes is one of the most common conditions in the American health care system. Estimates for the lifetime incidence of diabetic foot ulceration is between 19% and 34% of all patients with diabetes. The global prevalence of diabetic foot ulcers is 6.4%, with male patients and older adults being the most likely to be affected. Foot ulcers often occur due to several factors working in conjunction, including arterial insufficiency and neuropathy. These conditions predispose a patient to lower extremity injuries that may result in an ulcer.1
Deficient sweating and altered perfusion in the foot can lead to dry skin that is easily injured with repetitive or minimal trauma. And the loss of sensation makes patients with diabetes vulnerable to foot trauma. Other diabetes-related conditions, such as defective white-cell function, also impair healing and enable the perpetuation of ulcers and the risk of infection.
Diabetic foot ulcers often occur in patients with neuropathy, necessitating frequent foot and leg examinations. Diabetic foot ulcers frequently occur on the plantar aspect of the foot, the tip of the toe, and lateral to the fifth metatarsal. These wounds are often deep, surrounded by callus, and insensate.1 Foot ulcer risk increases in patients with a past or current history of foot ulcer, gangrene, or lower-limb amputation.
Living with a Lower Extremity Wound
While the etiology of these different lower extremity wounds vary, the impact on the patient is often similar. Symptoms may include:
- Pain, particularly in chronic wounds. Between 48% to 81% of patients with chronic lower extremity wounds report moderate to severe pain.
- Psychosocial impacts may be wide-ranging and include diminished confidence in appearance, dignity, and self-perception. Patients may limit social interaction due to wound symptoms that include exudate and odor. Many patients also report a change in their sex life or libido. Anxiety and depression commonly accompany chronic pain when it is not managed sufficiently.
- Limited mobility due to the wound itself or its accompanying pain can make it hard to complete daily tasks and retain gainful employment.9
- Care of the wound, including managing exudate and odor, is difficult. Frequent dressing changes can be challenging and painful for patients with lower extremity wounds.10
Ultimately, life for patients with lower extremity wounds is often severely impacted. The physical damage to the body is one impact, but the complications that decrease the quality of life and present care challenges make living with these wounds even harder.
Treating Lower Extremity Wounds
Since living with a lower extremity wound presents many physical, emotional, and psychological hardships, the goal is to implement care strategies that accelerate wound closure and minimize the effects of chronic wounds. Despite the differing etiologies of lower extremity wounds, many of the treatment strategies are beneficial for all types of wounds, including:
- Regular limb assessments to identify early warning signs of a problem. If a wound is present, it should be assessed on many dimensions, including the conditions of the skin, current vascular status, shape and size, and the history, location, and status or stage of the ulcer.
- Patient education must include identifying and mitigating risk factors, making lifestyle changes to reduce the risk, and understanding the importance of ambulation, offloading, or other treatment strategies.
- Clinicians should also educate patients on the necessity of proper footwear and the importance of routine foot hygiene, including regularly inspecting the foot, clipping the nails, and cleansing the area.
- Compression therapy can be considered when clinically indicated, although this treatment is not recommended on ischemic wounds or with congestive heart failure patients.
- The use of advanced wound care modalities, such as negative pressure wound therapy, can be beneficial in wounds that have excess exudate or those with a high risk of becoming infected. Hyperbaric oxygen therapy, electrical stimulation, and surgical interventions may also be considered depending upon the unique characteristics of the patient and the contributing factors of their underlying disease.
- The selection of optimal dressings can help manage exudate and maintain moist healing conditions, promoting faster wound closure.
- The use of a strong but gentle medical adhesive can protect the ulcer while it is healing and maintain the integrity of the periwound area.
How Hy-Tape Can Help
As a leading provider of medical adhesives, Hy-Tape offers gentle medical adhesives that can secure dressings and help protect lower extremity leg wounds while they heal. Hy-Tape products are ideal for protecting fragile, sensitive, and healing skin. Hy-Tape products are nurse-approved, and in a recent study, were frequently rated as “Excellent” by health care practitioners.
Hy-Tape is Gentle. With a zinc-oxide base, Hy-Tape is soothing to delicate skin and prevents irritation and damage to sensitive, broken, or inflamed skin. The adhesion is non-reactive and easily removable. This trait ensures that the dressings will hold tight but release gently, reducing the risk of irritation on sensitive and healing skin.
Hy-Tape is Non-reactive and Latex-Free. Patients with sensitive or dry skin – as is common in the periwound area of many lower extremity wounds – will appreciate that Hy-Tape products are non-reactive and latex-free, ensuring that they won’t cause further irritation.
Hy-Tape Helps to Maintain a Moist Healing Environment. Exudate management is one of the most difficult aspects of caring for a lower extremity wound. Hy-Tape products are waterproof, so they won’t loosen or come off in the presence of excess exudate, helping to keep your dressings in place.
Hy-Tape is Strong. Hy-Tape products are gentle yet strong enough to prevent contaminants, such as exudate, stool, or urine, from reaching the wound. This feature ensures that already-fragile skin will remain protected. It also helps to reduce the risk of infection, inflammation, delayed wound healing, gangrene, and amputation.
Conclusion
Lower extremity wounds are becoming increasingly common, and they often come with a host of complications. They are complex, prone to infection, multifactored wounds that often become chronic. Moreover, the prevalence of these wounds is increasing due to many contributing factors in the modern lifestyle. Patients with arterial, venous, or diabetic ulcers often live in perpetual pain with a diminished quality of life. Selecting a waterproof and gentle adhesive to secure dressings and therapeutic devices can enhance the healing environment – which is one component of creating optimal healing conditions and achieving wound closure.
The use of Hy-Tape products is one part of improving the standard of care for these wounds. Adhering to other wound care best practices, in conjunction with gentle adhesives, tapes, and dressings is essential in achieving better patient outcomes that can promote an enhanced quality of life for patients with these wounds.
To learn more about how Hy-Tape can help optimize treatment of lower extremity wounds, contact one of our representatives or visit
REFERENCES:
1. Singer J, Tassiopoulos A, Kirsner RS. Evaluation and management of lower-extremity ulcers. N Engl J Med. 2017;377(16):1559-1567.
2. Pugliese DJ. Infection in venous leg ulcers: considerations for optimal management in the elderly. Drugs Aging. 2016;33(2):87-96.
3. Harnarayan P, Ramdass MJ, Maharaj R, Naraynsingh V. Types of ulcers of lower extremity. In: Khanna AK, Tiwary SK (eds). Ulcers of the Lower Extremity. New Delhi, India: Springer India; 2016:15-38.
4. Luz AR, de Souza Pereira da Silva MC, de Moura Vergara R, Mourao MSF. Lower limb ulcers. In: Navarro TP, et al. (eds). Vascular Diseases for the Non-Specialist. Cham, Switzerland: Springer International; 2017:203-220.
5. Meda N, Abbas M, Tripathi RK. Arterial ulcer. In: Khanna AK, Tiwary SK (eds). Ulcers of the Lower Extremity. New Delhi, India: Springer India; 2016: 163-179.
6. Armstrong DG, Boulton AJM, Bus SA. Diabetic foot ulcers and their recurrence. N Engl J Med. 2017;376(24):2367-2375.
7. Pengzi Z, Jing L, Yali J, Sunyinyan T, Dalong Z. Global epidemiology of diabetic foot ulceration: a systematic review and meta-analysis. Ann Med. 2014;49(2):106-116.
8. Al-Rubeaan K, Derwish MA, Ouizi, S, et al. Diabetic foot complications and their risk factors from a large retrospective cohort study. Plos One. 2015;10(5):e0124446. doi:https://doi.org/10.1371/journal. pone.0124446
9. Edwards H, Finlayson K, Skerman H, et al. Identification of symptom clusters in patients with chronic venous leg ulcers. J Pain Symptom Manage. 2014;47(5):867-875.
10. Platsidaki E, Kouris A, Christodoulou C. Psychosocial aspects in patients with chronic leg ulcers. Wounds. 2017;29(10): 306-310.
11. Newbern S. Identifying pain and effects on quality of life from chronic wounds secondary to lowerextremity vascular disease: an integrative review. Adv Skin Wound Care. 2018;31(3):102-108.
12. LeBlanc K, Woo K, Christensen D, et al. Best practice recommendations for the prevention and management of skin tears. Wounds Canada. Canadian Association of Wound Care. 2018, updated
2021. https://www.woundscanada.ca/docman/public/health-care-professional/552-bpr-prevention-andmanagement- of-skin-tears/file. Accessed June 26, 2021.

