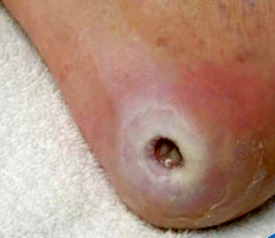
While a moist environment has been proven to help facilitate a healthy healing process, issues may arise that require attention. One of the more common issues that occurs when a dressing is left on too long or is not properly secured is macerated skin. Skin maceration happens when skin is in contact with moisture for too long which can lead to break down of the skin. When an overly aggressive adhesive is introduced to macerated skin, further damage will occur. Below is a background on skin maceration, warning signs, and ways to mitigate adhesive damage to peri-wound skin.
What causes skin maceration during wound healing?
Wound exudate – Moist wound healing is a proven method for producing a positive healing environment. It improved healing time, recedes pain and can reduce the chance of infection, However, when wound exudate is not properly managed, the skin may become macerated which can slow the healing process and even create a larger wound area.
Excessive sweating or hyperhidrosis – While it is a relatively rare condition (nearly 3% of the population), excessive sweating or hyperhidrosis without allowing the ski to breath will lead to the delayed healing, possible infection, discomfort, pain, and eventual skin breakdown.
Traditional and overly aggressive dressing adhesives and tapes – Skin stripping may occur as a result of repeated removal of traditional wound adhesives on over saturated skin surrounding the wound.
Improper dressing selection or weartime – Maceration is generally evident upon dressing removal (below are some signs of maceration to watch out for).
Incontinence – People with incontinence or who stay in bed for long periods of time due to a condition may experience skin maceration. Prolonged contact with urine-soaked clothing, incontinence pads, or bedsheets can lead to:
- Skin maceration
- Dermatitis
- Infections due to bacteria or fungus
Other causes of skin maceration include:
- Not changing the wound dressings at the proper frequency
- Bed rest without proper care with chronic and post surgical wounds
Signs of macerated per-wound skin
Maceration generally occurs when slow healing wounds like bed sores, ulcers, burns, and diabetic wounds are left wet too long. Some symptoms of skin maceration include, but are not limited to:
- An overly moist and spongy wound bed
- Pale, wrinkled white flesh surrounding the wound
- Red and irritated skin
- Increased pain and swelling
- Foul smelling discharge
Patients should report any of the above symptoms to their care professional.
Treatments for macerated skin and preventative measures
In many cases macerated wounds and peri-wound skin can be repaired by allowing fresh air to dry the skin with medical professionals guidance. Other methods to keep skin healthy in a moist wound environment include:
- Sterile gauze pads and wound pads and clearing the excess fluid
- Rinsing the wound with sterile water
- When needed, using a layer air antibiotic cream, Bacitracin, or Neosporin.
- Using a breathable bandage as a change of pace
- Frequent check-ups
Protecting the peri-wound from maceration
Per-wound breakdown generally occurs when the moisture from the wound bed infiltrates the healthy skin surrounding the wound by either secreting beneath the adhesive or when the adhesive itself causes damage to the skin. Skin protection is important when repeat dressing changes are needed to encourage healing. Hy-Tape is an excellent solution for securing dressings in moist wound healing environments for in areas where an airtight seal is needed. Hy-Tape is known for holding firm, while releasing gently and is especially suited for repeat applications. The adhesive in Hy-Tape contains zinc-oxide which is known to sooth irritated skin. If you would like to try Hy-Tape latex free take, please click here.

