Mature skin is not only more prone to damage than younger adult skin, but it also takes longer for older skin to heal. By the time we reach age 65, our skin cells replace themselves only about half as quickly as they did when we were younger.1 However, this article is not just another reminder of the long list of things that happen to us when we age. Quite the opposite; this article contains the information needed to fight back against the effects of aging skin and educate caregivers on wound care for older individuals.
Skin health is more than just a beauty contest
If anyone has ever asked you to guess their age, you no doubt looked at their skin for a clue. Our skin is usually a good indicator of age; smooth skin when we were a child, acne when we were a teenager, or an increasing number of wrinkles as aging adults. Dermal fillers, toxin injections, and face lifts help with the aesthetic issues of aging skin, but cosmetic procedures cannot reverse the structural and functional consequences of age. At a certain point—usually starting by age 70—the focus of skin care must change to one of skin health and health-related quality of life.2
Know your enemy – The causes of skin aging
A combination of external and internal processes cause skin to age. Ultraviolet (UV) light, smoking, and air pollution all accelerate the skin aging process. However, we can avoid most of the external factors that cause skin to age (e.g., wearing sunscreen). The natural, internal aging process is unavoidable. As we age, the amount of fat and moisture in our faces, hands, and feet naturally decreases leaving the overlying skin to dip and sag. The skin becomes thinner and more fragile with age, too, which makes the skin more prone to trauma.3 The thinning dermal layer becomes more rigid, less elastic, and highly prone to tearing.4 Even the physical connection between the layers of skin changes, which may be the biggest enemy of skin as we age.
Mature skin’s biggest enemy – MARSI
MARSI stands for medical adhesive-related skin injuries. MARSI occurs when the attachment of medical adhesives to the skin is stronger than the bonds between layers of skin or skin cells. Unfortunately, healthcare professionals are largely unaware of MARSI or appreciate how serious it can be.5 On the other hand, many older individuals and the healthcare professionals who care for them know MARSI very well, or at least MARSI’s effects on skin and health.
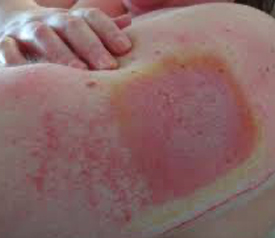
MARSI is associated with skin stripping, blistering, and tearing, and may leave skin irritated and macerated.5 Indeed, medical adhesives can literally tear the skin causing tremendous pain. The resulting skin damage can expand wounds, interfere with wound healing, or even cause new wounds. Every wound is a possible source of infection.6
Modern medical care would come to a halt if healthcare providers could not use medical adhesives like the adhesive found in medical tape. Unfortunately, many are associated with MARSI.5 While these products have an important place in medical care, most are designed with younger patients in mind. Older people deserve better. Fortunately, MARSI is entirely preventable.
Fighting back against MARSI
Mature patients and their caregivers can prevent MARSI by making small changes to their current products and processes.5 For example, the adhesive in paper and plastic surgical tapes often contain acrylate, which increases its adhesion over time.5 In most circumstances, surgical tapes should not be used on older patients, especially if the tape will be applied for more than a few hours. The tape adheres so tightly that it is increasingly likely to tear the skin when it is removed.
Silicone adhesives
Instead, silicone and zinc oxide adhesives offer better protection against MARSI.5 Silicone adhesives in medical tape are latex-free and moisture-resistant, but are less moisture-resistant acrylate tapes (they are also much more expensive). Silicone adhesives are gentle on skin, but they are not strong enough for some applications (e.g., securing critical tubing).5 On the other hand, because they release so easily, they can be repositioned and used for repeated applications.
Zinc oxide adhesives
Medical tape with zinc oxide adhesives—like Hy-Tape—may offer the best combination of safety, security, and cost. Unlike surgical tapes that contain acrylate, Hy-Tape’s zinc oxide adhesive does not adhere more aggressively over time. It releases cleanly and without traumatizing the skin. Hy-Tape is still gentle on mature skin even after a day or more of wear. So, while Hy-Tape adheres more securely than silicone-based adhesives, if removed properly it can be repositioned as needed. Thus, Hy-Tape can be used for many medical applications that silicone-based tapes cannot. Added to this, zinc oxide creates a barrier that helps the skin retain moisture and stay hydrated. Hy-Tape is also less expensive than silicone adhesive-based tapes overall. Therefore, Hy-Tape seems to be the ideal medical tape to serve the needs of mature patients while reducing their risk of MARSI.
Read more about MARSI and methods of prevention:
- Mitigating Medical Adhesive-Related Skin Injury (MARSI)
- Skin Tears & Securing Devices On Geriatric & Neonatal Patients
- Dressing Securement Strategies and Medical Adhesive-Related Skin Injuries
- Skin Tear Prevention
References
1. Goodson WH, 3rd, Hunt TK. Wound healing and aging. J Invest Dermatol. 1979;73(1):88-91. 10.1111/1523-1747.ep12532775
2. Farage MA, Miller KW, Elsner P, Maibach HI. Characteristics of the Aging Skin. Adv Wound Care (New Rochelle). 2013;2(1):5-10. 10.1089/wound.2011.0356
3. Ghadially R, Brown BE, Sequeira-Martin SM, Feingold KR, Elias PM. The aged epidermal permeability barrier. Structural, functional, and lipid biochemical abnormalities in humans and a senescent murine model. J Clin Invest. 1995;95(5):2281-2290. 10.1172/JCI117919
4. McCallion R, Li Wan Po A. Dry and photo-aged skin: manifestations and management. J Clin Pharm Ther. 1993;18(1):15-32. 10.1111/j.1365-2710.1993.tb00562.x
5. Fumarola S, Allaway R, Callaghan R, et al. Overlooked and underestimated: medical adhesive-related skin injuries. J Wound Care. 2020;29(Sup3c):S1-S24. 10.12968/jowc.2020.29.Sup3c.S1
6. Reinke JM, Sorg H. Wound repair and regeneration. Eur Surg Res. 2012;49(1):35-43. 10.1159/000339613

