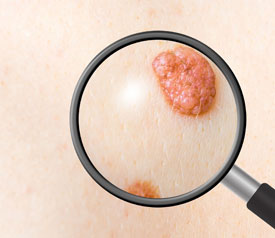
Actinic keratosis is not skin cancer, and most actinic keratoses do not become cancer. On the other hand, most squamous cell carcinomas (i.e., skin cancer) emerge from actinic keratoses. Since it is difficult to determine which actinic keratosis lesion will eventually become cancerous1, most are actinic keratoses are treated just in case. Proper skin care after actinic keratosis can help reduce the risk of scar formation and improve the cosmetic appearance.
Actinic keratosis treatments
People have many options for actinic keratosis treatment:
- Cryotherapy – The actinic keratosis lesion is frozen with liquid nitrogen, killing the cells within it. Cryotherapy is usually the preferred treatment for actinic keratosis because it is fast, well-tolerated, and does not require local anesthesia. However, the lesion cannot be tested after it is frozen, so cryotherapy is usually used when the actinic keratosis is almost certainly not cancerous. It may be followed up with a topical treatment like fluorouracil.
- Topical treatments – Topical treatments are placed on the actinic keratosis lesion to destroy it. Topical treatments for actinic keratosis include fluorouracil, imiquimod, ingenol mebutate, diclofenac, or tirbanibulin. Fluorouracil is widely used for actinic keratoses that are not very deep, especially on the face where the cosmetic result may be important. Unfortunately, treatment takes up to four weeks and during that time the skin is red, contains blisters, and develops erosions before healing.2
- Photodynamic therapy – A light sensitizing agent is applied to the skin and the area is treated with light (not laser) therapy. The combination of sensitizing agent and light destroys the lesion. Patients may or may not find this approach painful.
- Dermabrasion – The actinic keratosis lesion and the top layer of skin is “sanded” away. The procedure is painful and requires both conscious sedation and local anesthetic. Without the top layer of skin, the area is left red and raw afterwards. This actinic keratosis treatment is only appropriate for fair-skinned individuals since it can cause hypopigmentation (i.e., loss of pigmentation).
- Chemical peels – A medium-depth chemical peel is applied to the actinic keratosis lesion to destroy it. Patients may experience a burning sensation, skin peeling, and changes in the pigment of their skin. Scarring is rare, but possible.
- Laser resurfacing – A medical laser is used to destroy to actinic keratosis lesion. Ablation laser therapy is painful, so conscious sedation and local anesthetic are usually required. The area may be red, swollen and weep fluid for days to weeks after the procedure.
- Surgical removal – The actinic keratosis lesion is carefully cut away under local anesthesia and, occasionally, conscious sedation. The advantage of surgical removal of actinic keratosis is that the lesion can be sent to the lab for analysis to check for cancerous cells. As with any surgery that breaks the skin, there is a risk for scarring.
Skin care after actinic keratosis treatment is important
Regardless of the type of actinic keratosis treatment you choose, your outcome heavily depends on your skin care after treatment. In all of the treatments listed above, part of the skin is being destroyed. Most of that skin is actinic keratosis, but the surrounding, healthy will also be affected. Indeed, that remains under and around the actinic keratosis lesion will be vulnerable for days to weeks after actinic keratosis treatment.
Skin care tips after actinic keratosis treatment
Because the skin is vulnerable after actinic keratosis treatment, all patients should keep the area clean and covered during healing.
Clean the area, gently – Avoid harsh cleansers like glycolic acid, face scrubs, or alcohol-based cleansers until the area is fully healed. Instead, use a mild cleanser such as Dove soap and water or other mild cleanser.
Keep the area dry, mostly – Healing takes place fastest in a moist, not wet environment. If you notice the area is producing fluid–common after laser resurfacing–cover the area with a dressing that will wick up excess moisture. If the area is very dry or crusty–common after cryotherapy–the area may need a petroleum-based ointment prior to placing the dressing. Do not use lotions or makeup in that area.
Protect the area from the sun, completely – UV rays from the sun are the main cause of actinic keratosis3 but they are also a major factor in skin scarring after actinic keratosis treatment. Fluorouracil and the sensitizing agents used in photodynamic therapy can greatly increase the risk of sunburn and sun damage. Keep the area covered with dressings and medical tapes like Hy-Tape that offer SPF protection.
Tape the area, securely – The medical tape you use for actinic keratosis aftercare should provide SPF protection, hold securely, resist soiling, and release gently and cleanly. Hy-Tape may be the ideal medical tape for actinic keratosis aftercare since it provides all of these features. When combined with the appropriate dressing, Hy-Tape can protect the area from harmful UV radiation while keeping dressing in their precise place. Hy-Tape can be used after any actinic keratosis treatment from cryotherapy to topical treatment to surgical removal.
Learn more about how Hy-Tape can be beneficial to patients and caregivers post dermatological procedures.
- Skin Cancer, Mohs Surgery & Scars
- Caring for Cutaneous Lymphoma Lesions
- Reducing Your Risk of Developing a Basal Cell Carcinoma Scar
- Minimizing & Protecting Your Melanoma Scar from the Sun
- The Unexpected Benefits of Zinc Oxide Medical Tape
References
1. Criscione VD, Weinstock MA, Naylor MF, et al. Actinic keratoses: Natural history and risk of malignant transformation in the Veterans Affairs Topical Tretinoin Chemoprevention Trial. Cancer. 2009;115(11):2523-2530. 10.1002/cncr.24284
2. Weiss J, Menter A, Hevia O, et al. Effective treatment of actinic keratosis with 0.5% fluorouracil cream for 1, 2, or 4 weeks. Cutis. 2002;70(2 Suppl):22-29.
3. Leffell DJ. The scientific basis of skin cancer. J Am Acad Dermatol. 2000;42(1 Pt 2):18-22. 10.1067/mjd.2000.103340

